I spent my last week at Kanti with one of three surgical teams. The week started with outpatient clinic. This is a rather chaotic morning where the doctors sit at one long desk and the patients all pile into the room and queue to be seen. Once again, there is no such thing as patient confidentiality. Everyone peers over each other’s shoulders as each child is undressed and examined right there at the consult desk. However this is the norm in Nepal and even if I am slightly taken aback by this approach the patients and families (and doctors) are not at all worried, as this is how it has always been. I guess one benefit is that numerous people are educated at once, as a result of discussing a condition with one patient while everyone else listens in!
There was a huge variation in cases. Presentations range from urinary tract infections and hydroceles that could be dealt with by a GP to acute appendicitis, inguinal hernias and all sorts of congenital malformations. Any patients requiring surgery were promptly booked in for the next day – what waiting lists?! This was really great for me as I was only spending a week with the team but it meant I still got to have some patient follow through.
There were a couple of stand out cases from this clinic for me. One 17-month-old girl presented with labial adhesions due to poor hygiene. She was whisked into the procedure room where, thank goodness, there was some privacy. The doctor then proceeded to bluntly dissect the adhesions with no anaesthesia or pain relief. The poor girl was screaming and in obvious agony.
I usually never have any issues with surgery – I can be scrubbed in and on my feet for a five-hour long procedure with no worries. I don’t get queasy at the sight of intestines, infected wounds or big nasty open fractures. This girl’s screams of pain however left me feeling light headed and nauseous. I had to leave the room and sit down which didn’t really help due to the fact I could still hear her cries.
I felt utterly helpless. It was just so brutal to perform such a sensitive procedure with no analgesia what so ever. At home in New Zealand this girl would most likely have been put under general anaesthetic or at least heavy sedation. Here, she was forcibly held down by nurses and her parents.
One thing that has struck me since working here is how tolerant of pain the Nepali children are. I have seen IV lines put in, lumbar punctures performed and minor procedures carried out with no topical or local anaesthetic with not even a grizzle. I think this fact really brought home to me just how much pain this girl was in.
There was nothing I could do about it. That’s just how some things are done here. Never mind that fact this girl is never going to want to come near a hospital or doctor again and rightly so. I don’t doubt this girl’s screams may ring in my ears for a long time to come, I just hope I never have to bear witness to such a thing again.
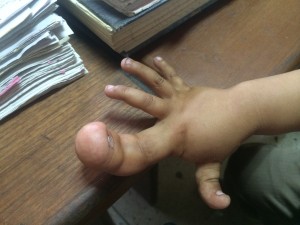
One of the more weird and wonderful cases I saw was a case of Macrodystrophia lipomatosa. This is a condition where the soft tissues of a couple of fingers or toes hypertrophy resulting in significant deformities. We had a four-year-old boy present with this in his left index finger and thumb (check out the photo!).It had been continuing to enlarge ever since he was a few months old. I always wonder with these cases why patients take so long to present – do they really think that it will spontaneously resolve? Unfortunately this case was referred on to the orthopaedic surgeons so I didn’t get to follow through and see what happened. From my reading on the condition surgery is the only option for treatment and include debulking and reconstruction procedures or amputation. Consideration is given to the amount of deformity; the level of disability and any significant nerve palsies or other anatomical complications. A very interesting case – I think one of those once in your career presentations!
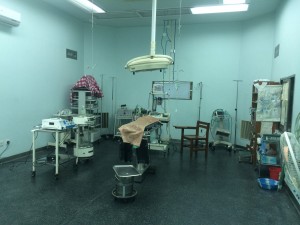
No surgical run is complete without a day in theatre. Kanti has two operating theatres (which face each other) and a minor ops area (which is located in the corridor). Patients walk into theatre past the minor ops table (where there is usually a patient midway through an operation), past the whiteboard with the list of patient names and procedures and into their theatre where they sit on the table and can look through the wide open doors into the next door theatre and see what is going on in there!
I really should be used to this no confidentiality thing already! None of this ever seems to faze the kids though and they happily jump onto the bed and lie down for the anaesthetist to put them to sleep. No parents there to comfort them or cool fairy/pirate apps on a smart phone to distract them. All just matter of fact; let’s get on with it.
I was reasonably impressed with the attempts to keep everything sterile. I probably did have reasonably low expectations to begin with though! There was the odd time where a surgeon would wipe his face on his sleeve though – that would potentially get you kicked out of theatre at home! All the instruments, drapes and gowns come sterilized and prior to admission the family buys any specialist equipment required.Many of the British medical students were shocked that the gowns were re-sterilized and not disposable but we have a similar system back in Christchurch so I wasn’t worried. That is until I spoke to another medical student who said that after being curious about the sterilization process he went on a bit of a mission. He found all the surgical gowns newly washed and “sterilized” drying on the ground on the roof of the hospital. I can only hope they have another sterilization process when they fold and pack them. Here’s hoping!!
 We had a reasonably busy day. The first two cases were two 56-day-old twins in for left inguinal hernia repairs. They had no identification bracelets and very similar names. Usually this would be a nightmare in a New Zealand hospital and there would be triple checks of patient identity and probably two time-outs before each operation just to make sure we were doing the right procedure on the right patient. I guess they figured since they were twins and both had the same presentation it wouldn’t really matter if there were a mix up! Luckily both operations went smoothly.
We had a reasonably busy day. The first two cases were two 56-day-old twins in for left inguinal hernia repairs. They had no identification bracelets and very similar names. Usually this would be a nightmare in a New Zealand hospital and there would be triple checks of patient identity and probably two time-outs before each operation just to make sure we were doing the right procedure on the right patient. I guess they figured since they were twins and both had the same presentation it wouldn’t really matter if there were a mix up! Luckily both operations went smoothly.
I also saw a biopsy and colostomy formation for a suspected Hirschprung’s disease in a nine-month-old boy and a colostomy closure in a 14-month-old girl. This was the final reconstructive procedure for this girl who had had a high anorectal malformation with a complete cloaca. These congenital malformations are quite common in Nepal and it was great to see such a successful outcome in someone so young.
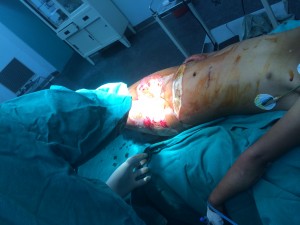
A debridement of 25% body surface area flame burns as a result of an all to frequent presentation with burns. Many families cook with either open fires or gas and the electrical system is very poorly maintained with loose wires and accidents are common.
The last case of the day was an 11-year-old male who had had a fever and rash for a week or so. He was found to have liver cysts on ultrasound so needed to have these drained. The boy was from the Terai (rural Nepal) and from a very poor family. They could not afford to keep him in hospital let alone buy the drains and other equipment required for the procedure. The doctors however found a solution. They added what was needed to the equipment lists of the 56-day-old twins, whose wealthy family promptly went out and purchased everything. Now they had two sets of equipment in case something went wrong while using the first lot!
My last day in Kanti was one of mixed emotions. I have thoroughly enjoyed my placement here and have seen and learnt about things I may never get the chance to come across in New Zealand. Yet it has also been quite harrowing at times. Dealing with any sick child can be emotionally difficult. It was even harder when so many were sick due to a lack of simple things like adequate food and proper hygiene.Seeing such poverty has made a massive impact on me. It changes your perspective on what is important in life and outlines how lucky we are to live in New Zealand. I only hope I never forget those lessons. So much has happened over the last three months that has had an impact on me both personally and professionally. Too much to put into words here at the end of this blog, so I plan to write one more in a week or so reflecting on my experiences. Hopefully you’ll stick around a bit longer for that.